 When certain parts of your brain receive specific patterns of messages, they respond by inducing pain, acting as a protective mechanism. This sensation signals that something might not be right, potentially indicating a threat to your health or safety. However, chiropractic care uniquely interprets these messages and facilitates a harmonious dialogue between your brain and body.
When certain parts of your brain receive specific patterns of messages, they respond by inducing pain, acting as a protective mechanism. This sensation signals that something might not be right, potentially indicating a threat to your health or safety. However, chiropractic care uniquely interprets these messages and facilitates a harmonious dialogue between your brain and body.
“Chiropractic helps your brain know what is going on in the spine and body,” said chiropractor Harvey Young.
At the core of our chiropractic treatment lies the understanding that the spine serves as a conduit for communication between the brain and the rest of the body. By ensuring proper alignment and function of the spine, chiropractors help your brain stay informed about your overall health status.
Chiropractic Helps Balance the Nervous System
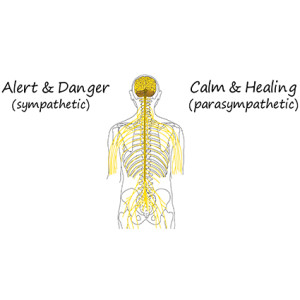 A fundamental aspect of the body’s communication network involves the sympathetic and parasympathetic nervous systems. When your body perceives a threat or danger, the sympathetic system kicks into high gear, triggering physiological responses such as increased heart rate, heightened alertness, and mobilisation of energy stores. This “fight or flight” response is essential for survival in threatening situations.
A fundamental aspect of the body’s communication network involves the sympathetic and parasympathetic nervous systems. When your body perceives a threat or danger, the sympathetic system kicks into high gear, triggering physiological responses such as increased heart rate, heightened alertness, and mobilisation of energy stores. This “fight or flight” response is essential for survival in threatening situations.
Conversely, the parasympathetic system, often called the “rest and digest” system, takes over when the danger subsides. It promotes relaxation, healing, and proper digestion, allowing your body to recuperate from the stresses of daily life. Chiropractic care helps to balance these two systems, ensuring that your body can effectively navigate between states of alertness and calmness as needed.
The Effects of Chiropractic Care on Brain Function
Recent scientific research has shed light on the profound effects of chiropractic care on brain function, particularly in the prefrontal cortex, a region responsible for orchestrating various cognitive functions. Studies have shown that chiropractic adjustments can alter the activity and function of this brain region, influencing the perception of pain and promoting overall wellbeing.
Activator Methods chiropractic care essentially fine-tunes the “music” playing in your brain by adjusting the spine and restoring proper function to the nervous system. It helps to modulate the signals that dictate your experience of pain, promoting a harmonious balance between alertness and relaxation. This alleviates discomfort and supports the body’s innate ability to heal and thrive.
Here is a resource and reference on “Pain is our Alarm System”:
Take That First Step Towards Relief
If you’ve been struggling with pain, we want to alleviate your discomfort naturally. Contact Harvey Young Advanced Holistic Therapy today to schedule an appointment with Harvey Young.
2. Brumagne S, Cordo P, Lysens R, et al. The Role of Paraspinal Muscle Spindles in Lumbosacral Position Sense in Individuals With and Without Low Back Pain. 2000;25(8):989-94. doi: 10.1097/00007632-200004150-00015
3. Szolcsanyi J. Effect of capsaicin on thermoregulation: an update with new aspects. Temperature (Austin, Tex) 2015;2(2):277-96. doi: 10.1080/23328940.2015.1048928 [published Online First: 2016/05/27]
4. Bohlen CJ, Julius D. Receptor-targeting mechanisms of pain-causing toxins: How ow? Toxicon: Official Journal of the International Society on Toxinology 2012;60(3):254-64. doi: 10.1016/j.toxicon.2012.04.336 [published Online First: 04/14]
5. Moller AR. Sensory systems: Anatomy and Physiology. California: Elsevier Science 2003.
6. Morasso P, Sanguineti V. Self-Organizing Body Schema for Motor Planning. Journal of Motor Behavior 1995;27(1):52-66. doi: 10.1080/00222895.1995.9941699
7. Lackner JR, DiZio P. Vestibular, Proprioceptive, and Haptic Contributions to Spatial Orientation. Annual Review of Psychology 2004;56(1):115-47. doi: 10.1146/annurev.psych.55.090902.142023
8. Kane MJ, Engle RW. The role of prefrontal cortex in working-memory capacity, executive attention, and general fluid intelligence: An individual-differences perspective. Psychon Bull Rev 2002;9(4):637-71. doi: 10.3758/bf03196323
9. Rossi AF, Pessoa L, Desimone R, et al. The prefrontal cortex and the executive control of attention. 2009;192(3):489-97. doi: 10.1007/s00221-008-1642-z
10. Haavik H, Kumari N, Holt K, et al. The contemporary model of vertebral column joint dysfunction and impact of high-velocity, low-amplitude controlled vertebral thrusts on neuromuscular function. European Journal of Applied Physiology 2021:1-46.
11. Lelic D, Niazi IK, Holt K, et al. Manipulation of dysfunctional spinal joints affects sensorimotor integration in the prefrontal cortex: a brain source localization study. Neural Plasticity 2016;2016
12. Apkarian AV, Bushnell MC, Treede R-D, et al. Human brain mechanisms of pain perception and regulation in health and disease. European journal of pain 2005;9(4):463-84.
13. Koyama T, McHaffie JG, Laurienti PJ, et al. The subjective experience of pain: Where expectations become reality. Proceedings of the National Academy of Sciences 2005;102(36):12950-55. doi: 10.1073/pnas.0408576102
14. Ploghaus A. Dissociating Pain from Its Anticipation in the Human Brain. Science 1999;284(5422):1979-81. doi: 10.1126/science.284.5422.1979
15. Wiech K. Deconstructing the sensation of pain: The influence of cognitive processes on pain perception. Science 2016;354(6312):584-87. doi: 10.1126/science.aaf8934 [published Online First: 2016/11/05]
16. Wager TD. Placebo-Induced Changes in fMRI in the Anticipation and Experience of Pain. Science 2004;303(5661):1162-67. doi: 10.1126/science.1093065
17. Loggia ML, Berna C, Kim J, et al. The lateral prefrontal cortex mediates the hyperalgesic effects of negative cognitions in chronic pain patients. The Journal Of Pain: Official Journal Of The American Pain Society 2015;16(8):692-99. doi: 10.1016/j.jpain.2015.04.003
18. Seminowicz DA, Moayedi M. The Dorsolateral Prefrontal Cortex in Acute and Chronic Pain. The Journal of Pain 2017;18(9):1027-35. doi: https://doi.org/10.1016/j.jpain.2017.03.008
19. Fenton BW, Shih E, Zolton J. The neurobiology of pain perception in normal and persistent pain. Pain Management 2015;5(4):297-317. doi: 10.2217/pmt.15.27 [published Online First: 2015/06/20]
20. Kimelberg HK, Nedergaard M. Functions of astrocytes and their potential as therapeutic targets. 2010;7(4):338-53. doi: 10.1016/j.nurt.2010.07.006
21. Apkarian AV, Hashmi JA, Baliki MN. Pain and the brain: specificity and plasticity of the brain in clinical chronic pain. Pain 2011;152(3 Suppl):S49.
22. Hadjistavropoulos TD, S; Goubert, L.; Mogil J.S.; Sullivan, M.J.L.; Vervoort, T.; Craig K.D.; Cano, A.; Jackson, P.L.; Rainville, P.; Williams, A.C.; Fitzgerald, T.D. A Biopsychosocial formulation of pain communication. Psychological Bulletin 2011;137(6):910- 39. doi: 10.1037/a0023876
23. Mitsi V, Zachariou V. Modulation of pain, nociception, and analgesia by the brain reward center. Neuroscience 2016;338:81-92. doi: 10.1016/j.neuroscience.2016.05.017
24. 24. Laird RA, Keating JL, Ussing K, et al. Does movement matter in people with back pain? Investigating ‘atypical’ lumbo-pelvic kinematics in people with and without back pain using wireless movement sensors. BMC Musculoskelet Disord 2019;20(1):28. doi: 10.1186/s12891-018-2387-x [published Online First: 2019/01/20]
25. 25. Cardinali DP. Autonomic Nervous System: basic and clinical aspects. Switzerland: Springer International Publishing 2017.
26. Kolb B, Whishaw IQ. BRAIN PLASTICITY AND BEHAVIOR. Annual Review of Psychology 1998;49(1):43-64. doi: 10.1146/annurev.psych.49.1.43
27. Hannibal KE, Bishop MD. Chronic Stress, Cortisol Dysfunction, and Pain: A Psychoneuroendocrine Rationale for Stress Management in Pain Rehabilitation. Physical Therapy 2014;94(12):1816-25.
28. Brown RA. Spinal Health: The Backbone of Chiropractic’s Identity. Journal of Chiropractic Humanities 2016;23(1):22-28. doi: https://doi.org/10.1016/j.echu.2016.07.002
29. McManus C. Chronic Stress, Chronic Pain, and the Corticolimbic System. Orthopaedic Physical Therapy Practice 2019;31(1):50-53.
30. Vachon-Presseau E. Effects of stress on the corticolimbic system: implications for chronic pain. Progress in Neuro-Psychopharmacology and Biological Psychiatry 2018;87:216-23. doi: https://doi.org/10.1016/j.pnpbp.2017.10.014
31. Melzack R. From the gate to the neuromatrix. Pain 1999;82:S121-S26. doi: 10.1016/s0304-3959(99)00145-1
32. Seymour B. Pain: A Precision Signal for Reinforcement Learning and Control. Neuron 2019;101(6):1029-41. doi: 10.1016/j.neuron.2019.01.055 [published Online First: 2019/03/22]
33. Sjøogaard G, Lundberg U, Kadefors R. The role of muscle activity and mental load in the development of pain and degenerative processes at the muscle cell level during computer work. European Journal of Applied Physiology 2000;83(2-3):99-105. doi: 10.1007/s004210000285
34. Butler D, Moseley AM. Explain Pain. 2 ed: Noigroup Publications 2013.
35. Ruddock JK, Sallis H, Ness A, et al. Spinal manipulation vs sham manipulation for nonspecific low back pain: a systematic review and meta-analysis. Journal of Chiropractic Medicine 2016;15(3):165-83.
36. Goertz C, Pohlman K, Vining R, et al. Patient-centered outcomes of high-velocity, low-amplitude spinal manipulation for low back pain: a systematic review. Journal of Electromyography and Kinesiology 2012;22(5):670-91.
37. Hidalgo B, Detrembleur C, Hall T, et al. The efficacy of manual therapy and exercise for different stages of non-specific low back pain: an update of systematic reviews. Journal of Manual & Manipulative Therapy 2014;22(2):59-74.
38. Paige NM, Miake-Lye IM, Booth MS, et al. Association of spinal manipulative therapy with clinical benefit and harm for acute low back pain: systematic review and meta-analysis. Jama 2017;317(14):1451-60.
39. Bryans R, Decina P, Descarreaux M, et al. Evidence-based guidelines for the chiropractic treatment of adults with neck pain. Journal of manipulative and physiological therapeutics 2014;37(1):42-63.
40. Wong JJ, Shearer HM, Mior S, et al. Are manual therapies, passive physical modalities, or acupuncture effective for the management of patients with whiplash-associated disorders or neck pain and associated disorders? An update of the Bone and Joint Decade Task Force on Neck Pain and Its Associated Disorders by the OPTIMa collaboration. The Spine Journal 2016;16(12):1598-630.
41. Gross A, Miller J, D’Sylva J, et al. Manipulation or mobilisation for neck pain: a Cochrane Review. Manual therapy 2010;15(4):315-33.
42. Bryans R, Descarreaux M, Duranleau M, et al. Evidence-based guidelines for the chiropractic treatment of adults with headache. Journal of manipulative and physiological therapeutics 2011;34(5):274-89.
43. Rist PM, Hernandez A, Bernstein C, et al. The impact of spinal manipulation on migraine pain and disability: a systematic review and meta‐analysis. Headache: The Journal of Head and Face Pain 2019;59(4):532-42.
44. Fernandez M, Moore C, Tan J, et al. Spinal manipulation for the management of cervicogenic headache: A systematic review and meta‐analysis. European Journal of Pain 2020;24(9):1687-702.
45. Schutze R, Rees C, Slater H, et al. ‘I call it stinkin’ thinkin”: A qualitative analysis of metacognition in people with chronic low back pain and elevated catastrophizing. British journal of health psychology 2017;22(3):463-80. doi: 10.1111/bjhp.12240 [published Online First: 2017/04/05]
46. Booth J, Moseley GL, Schiltenwolf M, et al. Exercise for chronic musculoskeletal pain: A biopsychosocial approach. Musculoskeletal care 2017;15(4):413-21. doi: 10.1002/msc.1191 [published Online First: 2017/04/04]
47. O’Connor SR, Tully MA, Ryan B, et al. Walking exercise for chronic musculoskeletal pain: systematic review and meta-analysis. Archives of physical medicine and rehabilitation 2015;96(4):724-34.e3. doi: 10.1016/j.apmr.2014.12.003 [published Online First: 2014/12/23]
48. Masino SA, Ruskin DN. Ketogenic diets and pain. Journal of child neurology 2013;28(8):993-1001. doi: 10.1177/0883073813487595 [published Online First: 2013/05/18]
49. Silva AR, Bernardo A, Costa J, et al. Dietary interventions in Fibromyalgia: a systematic review. Annals of medicine 2019:1-29. doi: 10.1080/07853890.2018.1564360 [published Online First: 2019/02/09]
50. Burgess HJ, Burns JW, Buvanendran A, et al. Associations Between Sleep Disturbance and Chronic Pain Intensity and Function: A Test of Direct and Indirect Pathways. The Clinical journal of pain 2019 doi: 10.1097/ajp.0000000000000711 [published Online First: 2019/03/27]
51. Goertz CM, Pohlman KA, Vining RD, et al. Patient-centered outcomes of high-velocity, low-amplitude spinal manipulation for low back pain: a systematic review. J Electromyogr Kinesiol 2012;22(5):670-91. doi: 10.1016/j.jelekin.2012.03.006 [published Online First: 2012/04/27]
52. Ruddock JK, Sallis H, Ness A, et al. Spinal Manipulation Vs Sham Manipulation for Nonspecific Low Back Pain: A Systematic Review and Meta-analysis. J Chiropr Med 2016;15(3):165-83. doi: 10.1016/j.jcm.2016.04.014 [published Online First: 2016/09/24]